Acid reflux is a very common occurrence. Many people experience this from time to time, and it generally brings no other side effects besides mild discomfort. However, chronic and persistent instances of acid reflux can point to gastroesophageal reflux disease, in which discomfort and irritation become common. In this post, we will be going over some of the various aspects of acid reflux and GERD, and be sure to contact AGH of Greater Washington with any questions you may have.
What Is Acid Reflux?
Acid reflux is when acid from your stomach moves back up into your esophagus. This occurs when the lower esophageal sphincter weakens or doesn’t tighten properly at the presence of food passing through it. Acid reflux causes heartburn as the main symptom, but it can also lead to other symptoms including a cough, sore throat, bitter taste in the mouth or throat, a sour taste in these areas, and burning pressure in the chest and stomach.
What Is Gastroesophageal Reflux Disease?
Gastroesophageal Reflux Disease (GERD) is also known as the chronic version of acid reflux. Frequent backflow of stomach acid into the lining of the esophagus creates backwash that irritates the lining of the esophagus. GERD is diagnosed when mild acid reflux occurs more than twice a week, severe acid reflux occurs at least once a week, or inflammation in the esophagus itself occurs frequently. Long-term esophagus damage can lead to forms of cancer.
What Causes Gastroesophageal Reflux Disease?
Simply put, chronic and frequent instances of acid reflux causes GERD. When you swallow, a band of muscle at the bottom of your esophagus relaxes to let food and liquid flow into the stomach. Once the substances pass through the esophagus, the band of muscle (sphincter) closes back up.
If this sphincter is weak or relaxed during this process, stomach acid can flow back up into the esophagus. The continued backwash of stomach acid irritates and inflames the esophagus, leading to acid reflux.
What are the Symptoms of Gastroesophageal Reflux Disease?
Common symptoms of GERD include:
- Heartburn
- Especially after eating and at night
- Chest Pain
- Difficulty Swallowing
- Regurgitation of Food and Sour Liquid
- Lump in the Throat
Common symptoms of nighttime GERD include
- Chronic Cough
- Laryngitis
- New or Worsening Asthma
- Disrupted Sleep
Risk Factors Associated With Gastroesophageal Reflux Disease
Risk factors that can increase your risk of GERD include:
- Obesity
- Bulging at the Top of the Stomach (Hiatal Hernia)
- Pregnancy
- Connective Tissue Disorders
- Delayed Stomach Emptying
Factors that aggravate symptoms of GERD include:
- Smoking
- Eating Large Meals or Late Night Meals
- Eating Trigger Foods like Fatty of Fried Meals
- Drinking Alcohol
- Drinking Coffee
- Certain Medications, Such as Aspirin
Diagnosing Gastroesophageal Reflux Disease
Your doctor or physician might be able to diagnose GERD from a physical examination and history of your signs and symptoms. Once they have speculated that GERD might be the cause of all the issues, they can confirm with several different tests.
- Upper Endoscopy
- A tube with a light and camera is inserted into the mouth and down the esophagus, detecting any inflammation or other complications.
- Ambulatory Acid Probe Test
- A monitor is placed in the esophagus to identify stomach acid regurgitation. The monitor connects to a small computer on the wrist, and after a few days of analysis, the monitor is passed out of the body in the stool.
- Esophageal Manometry
- Measures the muscle contractions, including coordination and force, of the esophagus while swallowing.
- Upper Digestive System X-Ray
- Taken in conjunction with a chalky liquid to gather a silhouette of the esophagus and stomach lining to analyze potential issues.
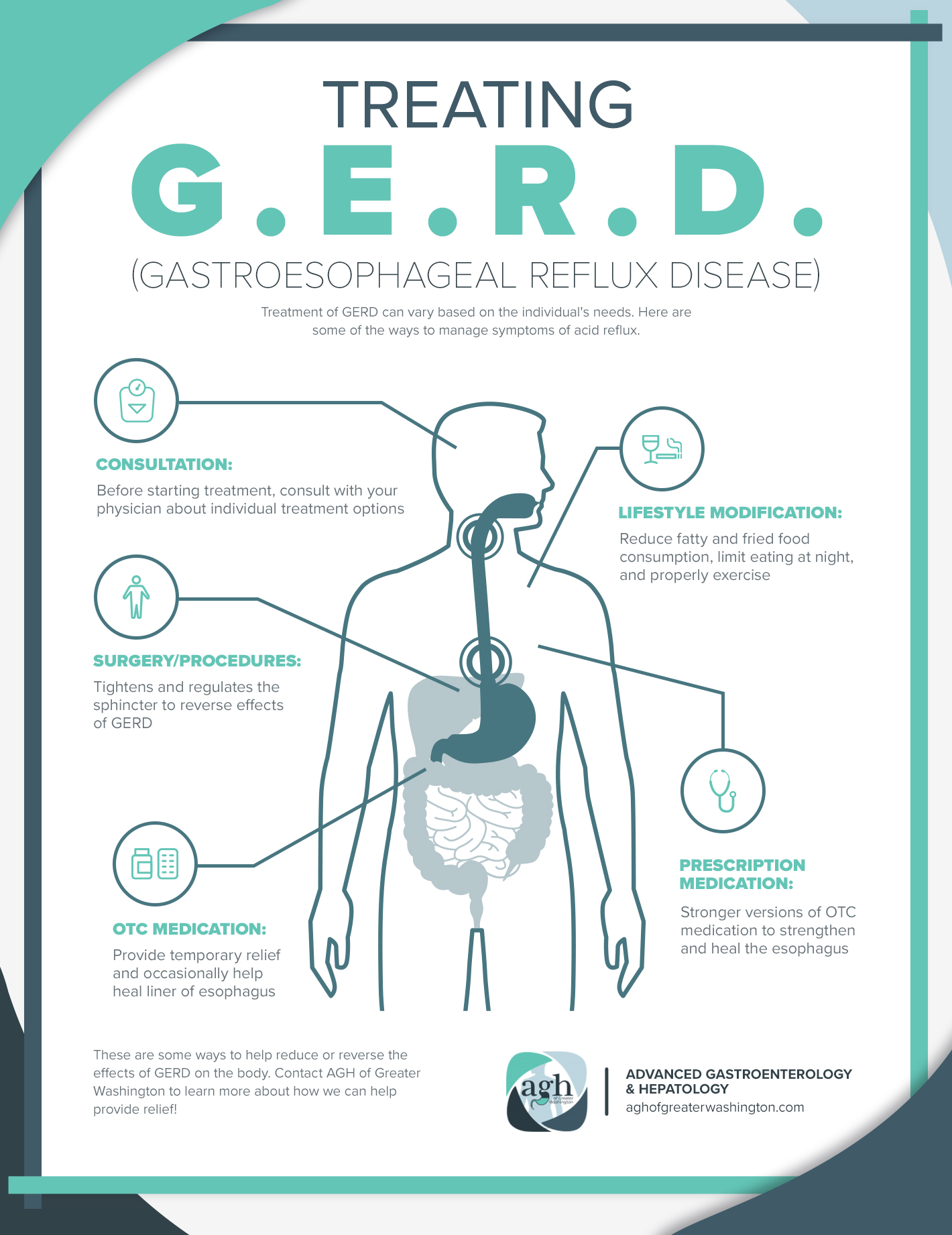
Treatment of Gastroesophageal Reflux Disease
Treatment for GERD varies depending on the person and the progression of the disease. Treatment can range from lifestyle changes to surgery depending on the situation and case.
Lifestyle Changes
Lifestyle changes that can help reduce the presence of GERD include a healthy diet and exercise. This includes cardiovascular exercise, the reduction of fatty or fried foods, and limiting eating that occurs at night.
Over-The-Counter Medications
These medications can be purchased on your own accord without a prescription, though it is wise to consult with your physician before beginning OTC treatment.
- Antacids that neutralize stomach acid
- These include Mylanta, Rolaids, and Tums. These will not heal a damaged esophagus but provide relief in the short-term.
- Medications that reduce acid productions
- Longer to kick in, but provide longer relief (up to 12 hours)
- Medications that block acid production and heal the esophagus
- Includes Prilosec OTC
Prescription Medication
- H-2 Receptor Blockers
- Proton Pump Inhibitors
- Strengthen Esophageal Sphincter
Surgery
- Fundoplication
- Minimally invasive, stomach wraps around sphincter to tighten the muscle
- LINX Device
- Magnetic beads keep the junction closed but allow food to pass through
- Transoral Incisionless Fundoplication (TIF)
- Polypropylene fasteners hold the junction together in this newer procedure
GERD Relief With AGH of Greater Washington
While GERD and acid reflux can inhibit your quality of life, you do not have to suffer alone. AGH of Greater Washington can provide treatment and services to help you in your journey. Contact our offices today to see how we can assist you!
Have questions? Fill out the form below!
The information AGH supplies on this website should not be used as a substitute to your regular physician’s medical advice. Your research from this website should not be used as a medical diagnosis. Consult your regular physician for diagnoses and treatments. The information found on this website is for educational purposes only. A formal consultation with a surgeon or doctor is needed before pursuing surgical procedures or medical treatments. Individual results may vary.
Gastroenterology Articles
Revitalizing Your Wellness with NAD+ Injections
Nicotinamide Adenine Dinucleotide (NAD+) is a cornerstone of cellular health, playing a vital role in energy production and DNA repair. As we age, our natural levels of this essential coenzyme decline, often leading to fatigue and reduced mental clarity. We are proud to offer specialized NAD+ therapy to help our patients reclaim their vitality and…
Navigating Chronic Liver Disease: Expert Hepatology Solutions
Dealing with a chronic liver condition can feel overwhelming, but our team is here to provide the specialized guidance and medical expertise you deserve. We focus on a multidisciplinary approach to hepatology, ensuring that every patient receives a tailored plan. By combining advanced technology with compassionate care, we help our community manage complex liver health…
Understanding Your Liver Health with Non-Invasive FibroScan® Technology
Monitoring liver health is a cornerstone of our commitment to your long-term wellness. As hepatology experts, we recognize that many liver conditions remain silent until they reach advanced stages. By utilizing cutting-edge diagnostic tools, we empower our patients with the knowledge needed to manage their health proactively and prevent the progression of chronic liver disease.…

